Far from isolated entities, our skin and gut harbour ecosystems of trillions of microscopic inhabitants known as the skin and gut microbiomes. These communities of bacteria, fungi, and even archaea play a crucial role in maintaining health and influencing a range of functions, from digestion and immunity to wound healing and skin barrier integrity.
Our skin hosts a diverse, dynamic microbiome shaped by factors like age, environment, medication and genetics. This delicate ecosystem functions as our first line of defence, producing antimicrobial substances and providing beneficial bacteria to fend off harmful disease-forming germs.
Within our digestive tract lies the gut microbiome, a more complex and diverse community with profound influences on our overall health. It regulates nutrient absorption, immune function, and even mood. Importantly, the gut microbiome communicates with the skin through an intricate network dubbed the gut-skin axis, sending signals via chemical messengers, and even the immune system.
When we sustain an injury, the skin microbiome springs into action. Our normal skin bacteria, like staphylococci and corynebacteria, produce antimicrobial peptides, deterring potential disease-forming germs and facilitating wound healing. They also stimulate the production of pro-inflammatory messengers, crucial for initiating the healing process. However, this inflammatory phase needs to be tightly regulated to prevent excessive tissue scarring.
Here is where the gut microbiome steps in. Short-chain fatty acids (SCFAs) produced by gut bacteria, function as messengers, travelling through the bloodstream and reaching the skin. Once there, they stimulate the production of antimicrobials, strengthen the skin barrier, and control inflammation. This promotes smooth, efficient wound healing.
Both the skin and gut microbiomes play vital roles in protecting us from infections and disease. The skin acts as a physical barrier, while the gut microbiome regulates the immune system, influencing the production of antibodies and immune cells. Importantly, the gut-skin axis facilitates communication between these two systems, ensuring a coordinated response to germs that cause disease.
When the equilibrium of either the skin or gut microbiome is disrupted, known as dysbiosis, negative consequences can arise. Skin dysbiosis can manifest as conditions like eczema or acne, while gut dysbiosis can lead to digestive issues, inflammatory bowel disease, and even impact neurological health. Disruptions in the gut-skin axis can further aggravate these issues, hindering wound healing and weakening immune responses.
How to keep your microbiome healthy?
- Eat a diet rich in fibre and prebiotics to nourish beneficial gut bacteria:
- Prebiotics function as food for our beneficial gut bacteria, promoting their growth and strengthening the gut barrier. Load up on fibrous vegetables like artichokes, asparagus, broccoli, and leafy greens, as well as fruits like berries, apples, and pears. Whole grains like quinoa, oats, and brown rice also pack a prebiotic punch.
- Fermented foods are teeming with live probiotic bacteria, the superheroes of the gut. Yoghurt, kimchi, sauerkraut, and kombucha are all excellent sources, helping to restore gut balance, boost immunity, and potentially improve wound healing.
- Omega-3 fatty acids have potent anti-inflammatory effects, benefiting both the gut and skin. Fatty fish like salmon, tuna, and sardines are your best bet, but walnuts, flaxseeds, and chia seeds also offer plant-based sources.
- Garlic acts as a natural antibiotic, helping to combat harmful bacteria in the gut and potentially improving skin conditions like acne. Turmeric and ginger also have anti-inflammatory properties and are beneficial.
- Probiotics supplements, containing live beneficial bacteria, can also be helpful in certain cases.
- Avoid sugary foods and beverages, refined and processed carbs and excessive alcohol consumption as these disrupt the gut microbiome and weaken the gut barrier.
- Make sure you drink enough water. Water is best for thirst and is vital to keep your microbial allies flourishing.
- Maintain a healthy sleep-wake cycle as disrupted sleep leads to fluctuations in hormones, favouring the growth of pro-inflammatory bacteria and weakening the gut barrier. This echoes onto the skin manifesting as increased sensitivity, dryness and even acne breakouts.
- Get 7-8 hours of good sleep a night.
- Expose your skin (without SPF) to the early morning sunlight to reap the benefits of vitamin D production and skin barrier fortification. Avoid the harsh midday sun and prioritise shade or sun protection in the hottest part of the day.
- Exercise regularly to increase blood flow to the skin.
- Practise mindfulness through yoga or meditation to reduce stress.
- Reduce your exposure to blue light from screens at night. Blue light reduces the production of melatonin which not only disrupts sleep but accelerates the growth of harmful bacteria causing inflammation and imbalances in the gut microbiome. On the skin blue light impacts the production of melanin, our natural sunshield, leading to pigmentation issues, accelerated ageing, and leaving us more vulnerable to infections and inflammatory conditions on the skin.
- Use warm-toned LEDs with dimmer switches to create gentle ambient light at night.
- Banish the screens at least an hour before sleep.
- Prioritise natural light exposure in the day to regulate your circadian rhythm and nurture the microbiomes.
- Consider blue light filters on your devices or reading glasses.
- Avoid screens during mealtimes as blue light can also disrupt digestion and the gut microbiome’s activity.
- Avoid the overuse of alcohol-based hand sanitisers, disinfectants, and antibiotics. Both can disrupt the healthy microbiome on your skin and in your gut, respectively. Happily, the active ingredient in our Trifectiv Plus range, namely our non-toxic hypochlorous acid, is a discretionary anti-microbial and microbiome-friendly disinfectant.
Research on the skin-gut axis is rapidly evolving, offering exciting possibilities for the future of medicine. Targeted microbiome interventions, including personalised probiotics and prebiotics, hold promise for managing both skin conditions and gut disorders. Additionally, understanding the complex communication between these ecosystems could lead to novel therapies for conditions ranging from autoimmune diseases to allergies.
The intricate dance between the skin and gut microbiomes reveals a fascinating truth: our inner and outer worlds are profoundly interconnected. By looking after our microbial allies, we can unlock a potent force for health and resilience. This means we heal faster, can resist disease more effectively, and can achieve a level of well-being that resonates from within.
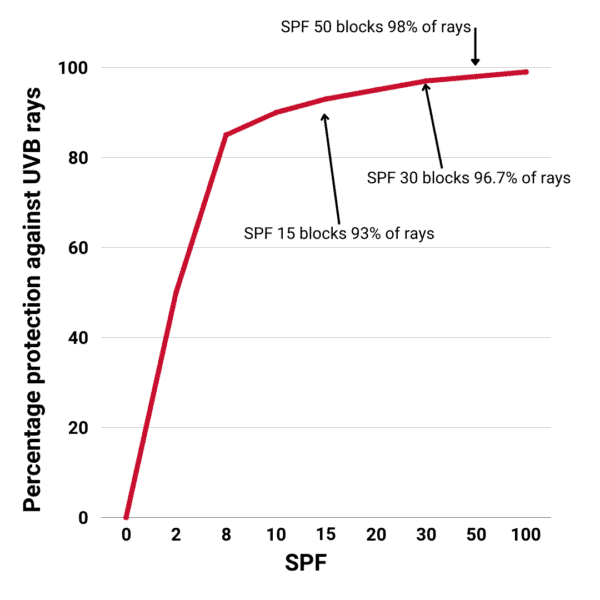
Some facts to consider when using SPF products.
- The chronic use of SPF is associated with a vitamin D deficiency. There is a growing awareness that this hidden danger needs to be added to the labelling requirements of SPF products.
- Sunscreens have not been shown to reduce the risk of melanoma or BCC. However, their use has been shown to reduce the risk of SCC.
- Studies have shown that the chemicals in sunblock appear in the blood in concentrations of up to 360 times more than what is considered safe by the FDA, after a single application. High circulating levels of sunblock chemicals can appear in the blood for up to 2 weeks after use and have been implicated in cases of kidney and liver failure.
- It is estimated that between 4,000 and 6,000 tonnes of sunblock ends up in the oceans every year! This chemical pollution has a devastating impact on the entire ecosystem, from algae and corals to fish and aquatic mammals.
- Physical or mineral sunscreens contain minerals that physically block harmful rays from the sun. The ingredients zinc oxide and titanium dioxide are found in mineral-based sunscreens. These are better choices for the ocean, but zinc oxide becomes toxic after two hours in the sun.
- Avoid spray-on sunscreen as they often contain chemicals that may damage the lungs.
- High-SPF sunscreens may give you a false sense of security and lead to more sunburn.
It therefore appears, in the face of recent research, that it is necessary to reconsider the current marketing strategy behind the multi-million-dollar industry of sun protection products. At the hottest time of the day, it is best to stay out of the sun in the shade or wear UV-protective clothing and a hat.
Recent advances in treating sunburn
The pathology associated with sunburn is UV-induced inflammation in the skin, which leads to structure and function breakdown, namely DNA-abnormalities in skin cells and accelerated ageing of the skin. Hypochlorous acid, a crucial component of our immune system and normally made by our white blood cells, is a powerful anti-inflammatory and also corrects the chromosomal abnormalities that occur with sunburn. Medical grade non-toxic hypochlorous acid, available as Trifectiv Plus Wound & Burn Care not only quickly calms and reverses sunburn, but also repairs the DNA damage associated with overexposure to UV radiation.
Closing thoughts
Achieving a balance between sun exposure and sun protection is essential for maintaining overall health. While excess sun exposure can lead to harmful consequences, avoiding the sun entirely may result in vitamin D deficiency and serious health risks. In the case of sun exposure, like being outside all day during a beach holiday, it is advisable to limit your exposure to the sun rather than using high-SPF products. Do not demonise the sun. Enjoy living in the outdoors but do this in moderation. If you are accidentally sunburnt then regularly apply Trifectiv Wound & Burn Care to reverse the associated inflammation. This will not only rapidly soothe the skin and ease any pain, but also assist the skin cells to heal any damaged DNA before it becomes a problem.
References
- Hoel DG, Berwick M, de Gruijl FR, Holick MF. The risks and benefits of sun exposure 2016. Dermatoendocrinol. 2016 Oct 19;8(1): e1248325. doi: 10.1080/19381980.2016.1248325. PMID: 27942349; PMCID: PMC5129901.
- Thomas H. Leung et al. Topical hypochlorite ameliorates NF-kB–mediated skin diseases in mice. J Clin Invest. 2013;123 (12):5361-5370 Stanford University School of Medicine, Stanford, California, USA
- Sunscreens leach up to 360 times more toxic chemicals into the blood than the FDA allows, raising the risk of kidney and liver failure. https://mol.im/a/7911979
- https://www.ewg.org/sunscreen/report/the-trouble-with-sunscreen-chemicals
- https://today.oregonstate.edu/news/osu-study-after-two-hours-sunscreen-includes-zinc-oxide-loses-effectiveness-becomes-toxic
- https://draxe.com/beauty/best-sunscreens/